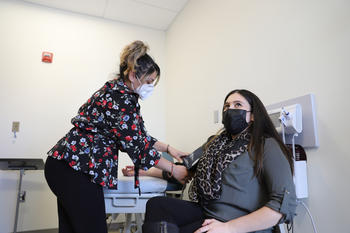
PMHNP students treat patients supervised by licensed practitioners at the only teaching clinic in the country for psychiatric medication management service that is affordable for all.

More than 50% of Americans will be diagnosed with a mental illness or disorder at some point in their lifetime, according to the Centers for Disease Control (CDC). In a given year, 20% will experience a mental illness. The ongoing pandemic has increased this by at least 10% percent, according to a CDC survey. Now nearly two years in, more people are seeking mental health support, however, finding a psychiatrist who is accepting new patients can be difficult and not always affordable.
Patients at Mason’s Center for Psychological Services (CPS) now have a new option— the Population Health Center’s behavioral health clinical services. Assistant Professor of Nursing Melanie Yousefi and the School of Nursing saw a need they could fill in the community plus a great way to train new psychiatric nurse practitioners and created this new program.
The College of Health and Human Services is sponsoring this new clinic which is the first-of-its-kind interprofessional clinic where Clinical Psychology doctoral students and Psychiatric-Mental Health Nurse Practitioner (PMHNP) students are delivering services in collaboration with each other and licensed faculty.
Training the Next Generation of Mental Health Professionals
With referrals from clinical psychology and counseling students at CPS, PMHNP students in the behavioral health clinic treat patients supervised by licensed practitioners on the College faculty. It is the only clinic in the country for psychiatric medication management service that is affordable for all and serves as an experiential learning environment for students.
“The clinic is providing hands-on psychological education for our PMHNP students,” said Yousefi, who is a certified PMHNP. “Most students can’t get this clinical experience anywhere else in the area until after they are certified. Because the clinic is part of an academic setting, there is more flexibility and our students get more real-world experience with real patients while still learning from the support of faculty members. They are able to receive feedback in real time to improve their practice and help the patient.”
PMHNP are licensed to diagnose mental health issues and to prescribe medicine as part of the treatment plan. All student clinical care is provided under direct supervision of Mason faculty who are experienced, practicing PMHNPs. Working with patients and PMHNPs, students learn by doing.
“I have had the experience of meeting clients from their initial evaluation, building rapport with them, and collaborating with them in such an important aspect of their health and overall wellbeing. It brings me great joy to join clients in attaining their mental health goals,” said Hiba Masood, a certified nurse practitioner and Mason PMHNP student. "I am honored to collaborate with the interprofessional team at the Center for Psychological Services, learning and growing with them and our mutual clients."
Students working in the clinic are experienced, licensed registered nurses enrolled in their clinical practicum and in the process of becoming a PMHNP and completing either their doctoral degree or post-master’s graduate certificate (if they are already an advanced practice nurse). Prior to their time at the Population Health Center, as with all Mason PMHNP students beginning their clinical practicum, nursing graduate students have already completed a wide range of mental health coursework including diagnostic training, psychotherapy, advanced pharmacotherapeutics, advanced physical health assessments, and psychopharmacology.
“Being a part of the teaching program with PHC has given me valuable clinical experience and helped to build my confidence and skills in providing quality care for clients," said Masood.
Interprofessional Collaboration for Well-Rounded Care and Education
“Mental health and physical health often coincide, and we are able to collaborate with CPS to provide the broad spectrum of mental health services to provide the best care for our patients,” said Yousefi. CPS provides evidence-based therapy and testing for clients of all ages in the community on a sliding scale, but it needed additional help with medication and pharmacology. Since fall 2021, CPS and the behavioral health clinic have worked together to provide complete patient mental health care.
CPS is a training clinic for doctoral students in clinical psychology that serves the Northern Virginia community on a sliding scale pay structure. Under the direction of Dr. Robyn Mehlenbeck, CPS has helped organizations and community members receive top-notch, evidence-based mental health care. CPS patients come from community referrals, including CPS’s emotional support phone line and Mason’s student services. However, the Center cannot provide medication or medication management, which is where the behavioral health clinic steps into patient care.
Behavioral health clinic patients, who are all referred from CPS, can see a PMHNP and receive prescriptions if needed. Previously, patients would have to go to outside community partners for this, and there was never any guarantee there were openings. Additionally, the two Mason clinics hold interprofessional meetings to discuss the best treatment for each patient. Students in both clinics are learning the scope of practice as students before they become licensed practitioners.
“This collaboration helps our students understand the complete process of psychopharmacology and psychotherapy treatment,” said Yousefi. “And the patient is receiving an overall wellness plan.” Mason is the only provider combining these two types of clinics and services to patients of any income.
Like CPS, Mason’s behavioral health clinic is a sliding scale model, which means the cost is income-based and affordable for those who have limited resources. No other training clinic in the country has a sliding scale for psychiatric medication management service, that Mason is aware of.
“It is wonderful to have the behavioral health services clinic as an on-campus partner,” said Mehlenbeck. “My trainee’s client started meds with Melanie’s team and reported he feels so much better. Accessible medication management is almost impossible to obtain, and yet, was exactly what this client needed. Working as an interprofessional team provides the best care to patients, the best training to our students and making this care accessible for our community is key.”
Next Steps for Growing the Clinic

“Melanie’s vision for this clinic is trailblazing for the College and the community. Two great teams are coming together to make health visible,” said interim Director of the School of Nursing Cheryl Oetjen. “We are grateful for the College’s support of this initiative, which has made it a reality.”
The behavioral health team is currently staffed to manage a limited caseload and hopes to be able to expand with additional funding. For every patient, only two students can assist one licensed practitioner so there are a limited number of appointments available. Since it is a training clinic, each visit takes twice as long as a standard doctor’s visit so that the students have time to understand what they are learning.
“Having more clinicians would allow for more availability to oversee care and student training, which in turn would allow for more referrals,” said Oetjen of the future of the clinic. When the clinic can support additional patients, Yousefi hopes to develop a referral process from the Mason and Partner (MAP) clinics too.
To further prepare students to serve in the clinic, Yousefi and Oetjen aim to work with the College’s Virtual Reality and Simulation Lab to do additional training with students before they start seeing patients in person. Mason will continue to prepare excellent mental health nurse practitioners to follow their passion for helping others.
“I enjoy being a great asset to the community,” said Masood. “It has been a privilege to be a part of launching this vital program for our community."
